DSM-5 SSD proposals
DSM-5 proposals
The material below is archived.
It predates the publication of draft proposals by the DSM-5 Somatic Symptom Disorders Work Group on February 10, 2010 (first draft); publication of the second draft on May 4, 2011 and publication of the third draft on May 2, 2012.
What changes has the DSM-5 Work Group for Somatic Symptom Disorders proposed so far?
[For ease of reference this material is being collated on one page.]
There is a degree of correspondence between the current Somatoform Disorders section in DSM-IV and the equivalent section in ICD-10: Chapter V. If the DSM-5 Task Force were to approve radical changes to its Somatoform Disorders categories, would ICD Revision still aim to achieve congruency between these sections of the two systems?
We have no information on how closely the ICD Topic Advisory Group for the revision of Chapter V: Mental and Behavioural Disorders (TAG MH) is collaborating with the DSM-5 Somatic Symptom Disorders Work Group over the revisions of their respective “Somatoform Disorders” sections.
Until the iCAT platform is launched and the ICD-11 Alpha Draft published (ETA May 2010), it is not apparent what changes TAG MH might be proposing for the structure, content and classifications of its corresponding Chapter V: F45 – F48 codes, or to what extent ICD Revision intends that any changes to its own “Somatoform Disorders” codings will mirror Task Force proposals for DSM-5.
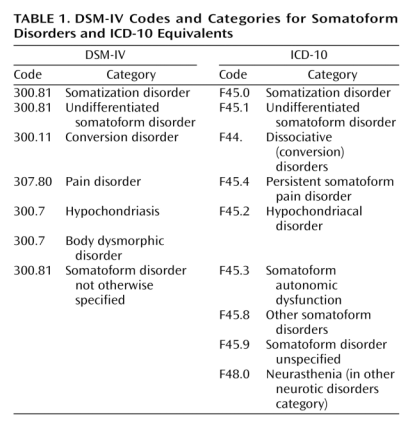
This table sets out how the two classification systems currently correspond for Somatoform Disorders.
Current DSM-IV Codes and Categories for Somatoform Disorders and ICD-10 Equivalents
Source: Mayou R, Kirmayer LJ, Simon G, Kroenke K, Sharpe M: Somatoform disorders: time for a new approach in DSM-V. Am J Psychiat. 2005;162:847–855.
This is the first report that the Somatic Symptom Disorders (aka Somatic Distress Disorders) Work Group published:
Report of the DSM-V Somatic Distress Disorders Work Group
November 2008
Joel Dimsdale, M.D.
This was followed, in April 2009, by this brief update:
Report of the DSM-V Somatic Distress Disorders Work Group
April 2009
Joel Dimsdale, M.D.
No further reports have been issued by the Somatic Symptom Disorders Work Group since April ’09, but an Editorial published in the Journal of Psychosomatic Research (for which SSD Work Group member, Francis Creed, is a co-editor) expands on the April report.
The Editorial: Dimsdale J, Creed F: The proposed diagnosis of somatic symptom disorders in DSM-V to replace somatoform disorders in DSM-IV – a preliminary report was published on behalf of the Somatic Symptom Disorders Work Group in the June ’09 edition of J Psychosom Res, 66 (2009) 473–476.
Read the free text on the Journal of Psychosomatic Research site
or Open the PDF here: Dimsdale Creed DSM-V SSD Work Group Editorial
Under the section “Psychological factor affecting a general medical condition”, towards the end of the Editorial, Dimsdale and Creed write that some authors have recommended wider use of this existing DSM-IV category as “a diagnosis that encompasses the interface between psychiatric and general medical disorders”, citing the Mayou R, Kirmayer LJ, Simon G, Kroenke K, Sharpe M paper: Somatoform disorders: time for a new approach in DSM-V. Am J Psychiat. 2005;162:847–855.
The Editorial reports that the [Psychological factors affecting a general medical condition] diagnosis “has been underused because of the dichotomy, inherent in the ‘Somatoform’ section of DSM-IV, between disorders based on medically unexplained symptoms and patients with organic disease”, and that by doing away with the “controversial concept of medically unexplained”, the proposed classification [Somatic Symptom Disorders] might diminish the problem.
The conceptual framework the Work Group was proposing, at that point:
“…will allow a diagnosis of somatic symptom disorder in addition to a general medical condition, whether the latter is a well-recognized organic disease or a functional somatic syndrome such as irritable bowel syndrome or chronic fatigue syndrome.”
The Editorial goes on to list a variety of different subtypes included within the diagnosis of “Psychological factors affecting a general medical condition” including a specific psychiatric disorder which affects a general medical condition; psychological distress in the wake of a general medical condition and personality traits or poor coping that contribute to worsening of a medical condition.
The authors suggest that these might be considered in the rubric “adjustment disorders” but that the location of this type of adjustment disorder had yet to be settled within the draft of DSM-5 and that the text and placement for these different variants of the interface between psychiatric and general medical disorders was still under review.
The authors conclude that the current structure proposed for DSM-V differed considerably from that of the somatoform disorders in DSM-IV; that the article gives an indication of a likely new structure, but that much remains to be done before this is finalised. The next steps would include defining the criteria for disorders and the relevant dimensions which may be used.
[Current use of the diagnosis “Psychological Factors Affecting Medical Condition” in DSM-IV is set out here ]
Several Letters to the Editor in response to this Editorial have been published in the Jan 2010 edition of J Psychosom Res and are referenced at the end of this posting; these require a subscription for access.
The recently published Editorial: Is there a better term than “Medically unexplained symptoms”? Creed F, Guthrie E, Fink P, Henningsen P, Rief W, Sharpe M and White P (Journal of Psychosom Research: Volume 68, Issue 1, Pages 5–8 January 2010) discusses the deliberations of the EACLPP study group. The Editorial also includes references to the DSM and ICD revision processes.
References to DSM and ICD revision in:
Is there a better term than “Medically unexplained symptoms”? J Psychoso Res: Volume 68, Issue 1, Pages 5–8.
[Extract]
Introduction
The European Association of Consultation Liaison Psychiatry and Psychosomatics (EACLPP) is preparing a [White paper of the EACLPP Medically Unexplained Symptoms study group by Peter Henningsen and Francis Creed] document aimed at improving the quality of care received by patients who have “medically unexplained symptoms” or “somatisation” [1]. Part of this document identifies barriers to improved care and it has become apparent that the term “medically unexplained symptoms” is itself a barrier to improved care…
…The authors of this paper met in Manchester in May 2009 to review thoroughly this problem of terminology and make recommendations for a better term….The deliberations of the group form the basis of this paper…
[…]
Our priority was to identify a term or terms that would facilitate management – that is it would encourage joint medical psychiatric/psychological assessment and treatment and be acceptable to physicians, patients, psychiatrists and psychologists.
Criteria to judge the value of alternative terms for “medically unexplained symptoms”
Ten criteria were developed in order to judge the value of potential terms which might be used to describe the group of symptoms currently referred to as medically unexplained symptoms. Obviously, this list of criteria does not claim to be exhaustive, but we believe that it captures the most important aspects. The criteria are that the term:
1. is acceptable to patients
2. is acceptable and usable by doctors and other health care professionals, making it likely that they will use it in daily practice.
3. does not reinforce unhelpful dualistic thinking.
4. can be used readily in patients who also have pathologically established disease
5. can be adequate as a stand alone diagnosis
6. has a clear core theoretical concept
7. will facilitate the possibility of multi-disciplinary (medical and psychological) treatment
8. has similar meaning in different cultures
9. is neutral with regard to aetiology and pathology
10. has a satisfactory acronym.Terms suggested as alternatives for “medically unexplained symptoms”
The group reviewed terms which are used currently or have been proposed for the future. An extensive list was abbreviated to the following 8 terms or categories: The terms we reviewed were:
1. Medically unexplained symptoms or medically unexplained physical symptoms
2. Functional disorder or functional somatic syndromes
3. Bodily distress syndrome/disorder or bodily stress syndrome/disorder
4. Somatic symptom disorder
5. Psychophysical / psychophysiological disorder
6. Psychosomatic disorder
7. Symptom defined illness or syndrome
8. Somatoform disorder[…]
Implications for DSM-V and ICD-11
There is overlap between the discussion reported here and the discussion currently under way towards the creation of DSM-V. Two of the authors (FC, MS) are also members of the working group on Somatic Distress Disorders of the American Psychiatric Association (APA), which is proposing a new classification to replace the DSM-IV “somatoform” and related disorders. In this working group, similar concerns about the use of the term and concept of “medically unexplained symptoms” have been raised [12]. The current suggestion by the DSM-V work group to use the term “Complex somatic symptom disorder” must be seen as step in a process and not as a final proposal. Unfortunately this term does not appear to meet many of the criteria listed above.
[…]
One major problem for reforming the classification relates to the fact that the DSM system includes only “mental” disorders whereas what we have described above is the necessity of not trying to force these disorders into either a “mental” or “physical” classification. The ICD-10 system has a similar problem as it has mental disorders separated from the rest of medical disorders.
The solution of “interface disorders”, suggested by DSM IV, is a compromise but it is unsatisfactory as it is based on the dualistic separation of organic and psychological disorders and prevents the integration of the disorders with which we are concerned here. This lack of integration affects the ICD classification also. For example functional somatic syndromes (e.g. irritable bowel syndrome) would be classified within the “physical” classification of ICD or Axis III in DSM (gastrointestinal disorders) and omitted from the mental and behavioural chapter entirely [13].
[End Extract]
DSM-5 presentations at The Academy of Psychosomatic Medicine Annual Meeting 2009
In November ’09, The Academy of Psychosomatic Medicine, publishers of Psychosomatics, held its 56th Annual Meeting in Nevada.
Three DSM-5 Work Group members, Francis Creed, Lawson Wulsin and Joel Dimsdale (Chair, Somatic Symptom Disorders Work Group) gave presentations around “Medically Unexplained Symptoms” (MUS) and DSM-5, and DSM-5 proposals. Slides are available, below, for the first two presentations, with text for the third.
This material represents the most recent information around the deliberations of the DSM-5 Work Group that is revising the categories currently under DSM-IV “Somatoform Disorders”.
Award Lectures
Hackett Award — Friday, 12:45pm – 1:45pm
Francis Creed, MD, FRCP: Can We Now Explain Medically Unexplained Symptoms?
[No transcript available]
Workshops
Workshop 15 — Saturday, 1:45 – 2:45pm
DSM-V for Psychosomatic Medicine: Current Progress and Controversies
Lawson Wulsin, MD, FAPM, DSM V for Psychosomatic Medicine: Current Progress and Controversies
[No transcript available]
Joel Dimsdale, MD, FAPM, Update on DSM V Somatic Symptoms Workgroup
[Text version of slides]
Update on DSM V Somatic Symptoms Workgroup
Workshop #15, APM Annual Meeting, 11-14-09
DSM-V for Psychosomatic Medicine: Current Progress and Controversies
Further references:
Journal of Psychosomatic Research, Volume 68, Issue 1, Pages 1-104 (January 2010)
Letters to the editor [subscription required]
The proposed diagnosis of somatic symptom disorders in DSM-V: Two steps forward and one step backward?
Andreas Schröder, Per Fink, pages 95–96
The concept of comorbidity in somatoform disorder—a DSM-V alternative for the DSM-IV classification of Somatoform disorder, Christina M. van der Feltz-Cornelis, Anton J.L.M. van Balkom, pages 97–99
The proposed diagnosis of somatic symptom disorders in DSM-V to replace somatoform disorders in DSM-IV—A preliminary report, 04 November 2009, Joel E. Dimsdale, Francis H. Creed, pages 99–10