October 20, 2011
by meagenda
Coding CFS in ICD-10-CM: CFSAC and the Coalition4ME/CFS initiative
Post #102 Shortlink: http://wp.me/pKrrB-1hd
Coalition4ME/CFS initiative

CFSAC discusses ICD-10-CM coding concerns
The Chronic Fatigue Syndrome Advisory Committee (CFSAC) provides advice and recommendations to the Secretary of Health and Human Services via the Assistant Secretary for Health of the U.S. Department of Health and Human Services (DHHS) on issues related to chronic fatigue syndrome (CFS).
Go here for the current Roster of Voting and Ex Officio committee members.
CFSAC holds twice yearly public meetings and meeting Agendas, Minutes, Meeting Materials, Presentations, Public Testimonies, Meeting Videocasts and CFSAC’s Recommendations to the DHHS are published on the CFSAC website.
The National Center for Health Statistics (NCHS), the Federal agency responsible for use of the WHO’s International Statistical Classification of Diseases and Related Health Problems, 10th revision (ICD-10) in the United States, has developed a clinical modification of the classification for morbidity purposes. The ICD-10 is used to code and classify mortality data from death certificates, having replaced ICD-9 for this purpose as of January 1, 1999.
The WHO has authorized the development of an adaptation of ICD-10 for use in the United States for U.S. government purposes. Although a U.S. specific adaptation, with U.S. committees and technical advisory panels responsible for its development and oversight, all modifications to the ICD-10 must conform to WHO ICD conventions.
ICD-10-CM is planned as the replacement for ICD-9-CM, volumes 1 and 2.
U.S. lags behind
While much of the world has been using the ICD-10 for many years and is looking to move onto ICD-11 (currently scheduled for implementation in 2015), the U.S. has been slow to make the transition from ICD-9-CM to a “clinical modification” of ICD-10.
ICD-10-CM development has been a long drawn out process and ICD-10-CM isn’t scheduled for implementation until October 1, 2013.
So when U.S. coders, clinicians, medical insurers and reimbursers are adapting to using ICD-10-CM, much of the rest of the world will be gearing up for ICD-11, which is planned to be a significantly different product to ICD-10, in terms of its structure, content, presentation, accessibility and its capacity, as an electronic publication, for continuous update and revision.
CFSAC new Recommendation to HHS
At the last CFSAC meeting (May 10-11, 2011), an hour long slot had been tabled on the agenda for Day One for discussion of concerns around the NCHS’s current proposals for the coding of CFS within ICD-10-CM.
The Committee was also informed of the considerable concerns for the implications for CFS and ME patients of the draft criteria and new categories being proposed by the DSM-5 “Somatic Symptom Disorders” work group.
A new CFSAC Recommendation to HHS was proposed by Committee member, Dr Lenny Jason, seconded by Dr Nancy Klimas, and voted unanimously in favour of by the Committee [1].
This new Recommendation, set out below, restates and expands on the Recommendation that CFSAC had made to HHS, in August 2005.
CFSAC rejects current proposals to code CFS in Chapter 18 of ICD-10-CM under R53.82: Chronic fatigue, unspecified > Chronic fatigue syndrome NOS. CFSAC continues to recommend that CFS should be classified in ICD-10-CM in Chapter 6 under “diseases of the nervous system” at G93.3, in line with ICD-10 and ICD-10-CA (the Canadian Clinical Modification), and in accordance with the Committee’s recommendations of August 2005. CFSAC considers CFS to be a multi-system disease and rejects any proposals to classify CFS as a psychiatric condition in US disease classification systems. (Note: no disease classification system under HHS’ control proposes to move or to include CFS in or among psychiatric conditions.) Source: CFSAC Recommendations – May 10-11, 2011
What are the current proposals?
For ICD-10-CM, the current proposals for the classification of PVFS and ME are:
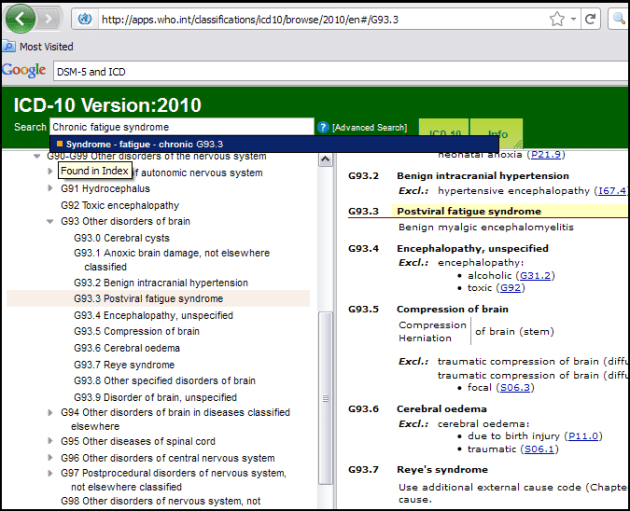
that Postviral fatigue syndrome would be classified within Chapter 6 Diseases of the nervous system under the parent class “G93 Other disorders of brain”, coded at G93.3.
(Benign) Myalgic encephalomyelitis would be classified as an Inclusion term under Title category “G93.3 Postviral fatigue syndrome”.
This is in keeping with the international ICD-10, from which ICD-10-CM has been developed. See Footnote [4] for link to page setting out current proposals for ICD-10-CM.
In ICD-10, Chronic fatigue syndrome is indexed to G93.3 in Volume 3 The Alphabetical Index.
In ICD-10-CA, the Canadian Clinical Modification of ICD-10, Chronic fatigue syndrome is classified in the Tabular List in Chapter 6, under “G93.3 Postviral fatigue syndrome”.
For ICD-11, the proposal is that all three terms should be classified within Chapter 6.
But for ICD-10-CM, instead of coding Chronic fatigue syndrome to G93.3, the proposal is to retain Chronic fatigue syndrome in the R codes chapter (which is Chapter 16 in ICD-9-CM and will be Chapter 18 in ICD-10-CM), where it would be coded thus:
Chapter 18 (Symptoms and signs and ill defined conditions)
[…]
R53.8 Other malaise and fatigue
R53 Malaise and fatigue
R53.82 Chronic fatigue, unspecified
Chronic fatigue syndrome (NOS)
Excludes1: postviral fatigue syndrome (G93.3)
(In ICD, NOS stands for “Not Otherwise Specified”.)
What is NCHS’s rationale for retaining CFS as (CFS NOS) in the R code chapter?
According to the background document Dr Wanda Jones presented to the Committee:
As it relates to CFS the use of two codes is consistent with the classification as there would be a code to capture CFS when the physician has determined the cause as being due to a past viral infection (G93.3) or if the physician has not established a link with a past viral infection (R53.82).
If code R53.82 were eliminated it would not be possible to disaggregate cases that are now distinguishable through the use of two codes.
There is a general equivalence map between ICD-9-CM and ICD-10-CM codes, however, if a concept is not carried over from the earlier version to the newer version data will be lost going forward.
Source: Extract: ICD-related questions from CFSAC for May 2011 meeting
Dr. Jones clarified for the Committee that if, in the clinician’s judgment, it was considered there is enough evidence to attribute the patient’s illness to a viral illness onset then the clinician could code to G93.3 (Postviral fatigue syndrome). If “however they could not identify where the trajectory developed toward CFS, then it would wind up in the R codes.” [1]
It has been further confirmed that testing for a viral illness is not required to assign a code – that coding is based on the clinician’s judgment.
And from the NCHS September 14 meeting
Proposals document:
In ICD-10-CM chronic fatigue syndrome NOS (that is not specified as being due to a past viral infection) was added to ICD-10-CM in Chapter 18 at R53.82, Chronic fatigue, unspecified. ICD-10-CM retained code G93.3 to allow the differentiation of cases of fatigue syndrome where the physician has determined the cause as being due to a past viral infection from cases where the physician has not established a post viral link. It should be noted that including chronic fatigue syndrome NOS at code G93.3 would make it difficult to disaggregate cases that are now distinguishable through the use of two separate codes.
Is this a new proposal?
No. This is a long-standing proposal that had been known about since at least 2007. It has been discussed on forums and raised in mailings on the Co-Cure Listserv list in 2007 and 2008 by U.S. advocates Mary Schweitzer and Jean Harrison, and flagged up by others in the U.S. and elsewhere, in the last couple of years.
The proposed coding of CFS, PVFS and (B) ME in the forthcoming ICD-10-CM had already been discussed at public CFSAC meetings in June 2004, when the NCHS’s, Donna Pickett, had given a presentation and again in September 2004, January 2005 and May 2010.
So the proposed coding of PVFS, (B) ME and CFS for ICD-10-CM is by no means a new issue.
As noted, ICD-10-CM has been under development for many years. A public comment period ran from December 1997 through February 1998. In 2001, the proposal had been that all three terms should be coded to G93.3, in keeping with the placement in the WHO’s ICD-10 [2].
I am advised that at one point, all three terms: PVFS, (B) ME and CFS, were proposed to be coded under G93.3, with a “CFS NOS” retained in the R codes. But that subsequently, the placement of CFS in Chapter 6 under the G93 parent class was deleted, leaving “CFS NOS” orphaned, in Chapter 18.
What is the ICD “R code” chapter for?
There is a four page ICD-11 Discussion Document that is worth a read: Signs and Symptoms [Considerations for handling categories and concepts currently found in chapter 18 of ICD-10, “SYMPTOMS, SIGNS AND ABNORMAL CLINICAL AND
LABORATORY FINDINGS NOT ELSEWHERE CLASSIFIED”, (R-codes), authors: Aymé, Chalmers, Chute, Jakob.] Open here: Discussion: Signs and Symptoms (Chapter 18)
The R codes chapter is the ICD chapter for “Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified (R00-R99)”
“This chapter includes symptoms, signs, abnormal results of clinical or other investigative procedures, and ill defined conditions regarding which no diagnosis classifiable elsewhere is recorded.” Source: ICD-10-CM Chapter 18, 2011 release.
Dustbin Diagnosis
At the May CFSAC meeting, Committee member, Steven Krafchick, a medical and disability attorney, raised his considerable concerns for the legal and medical insurance ramifications of coding CFS under the “R codes” at the May CFSAC meeting [1].
Coding CFS under R53.82 for “non viral onset” cases will consign patients to a dustbin diagnosis that will continue to confuse and conflate Chronic fatigue syndrome with Chronic fatigue. There are no certainties that clinicians will code new cases using the unfamiliar G93.3 PVFS and ME codes or that existing CFS patients will get “upgraded” to G93.3 ME.
Coding CFS under R53.82 under ill defined conditions will make patients more vulnerable to the proposals of the APA’s DSM-5 “Somatic Symptom Disorders” Work Group.
Coding CFS under R53.82 will render ICD-10-CM out of line with at least four versions of ICD-10, including Canada’s ICD-10-CA, which has all three terms classified in the Tabular List under G93.3, and out of line with proposals for the forthcoming ICD-11, scheduled for implementation in 2015. The U.S. would be the only country with CFS coded in the R codes.

Have representations been made to the NCHS Committee?
Although representations around the coding of CFS for ICD-10-CM have been made to CDC over the years, no stakeholder representations at NCHS meetings are recorded.
At the May CFSAC meeting, Dr Jones informed the Committee that the ICD-CM process is a public process and that there is an opportunity to input into the update of ICD-9-CM and development of ICD-10-CM as part of that process, and to engage with the NCHS Committee via regularly scheduled public meetings. Dr Jones confirmed that NCHS has stated that there has been no public presence from the CFS community at these meetings.
It was established during the May meeting that the deadline for submitting representations for new inclusions or modifications to existing proposals for ICD-10-CM for tabling for discussion at the next NCHS Coordination and Maintenance Committee meeting would close on July 15, for a meeting scheduled for September 14. It was further noted this would be the last meeting before implementation of the partial code freeze and that this was therefore a time sensitive issue.
Committee members discussed the potential for a representative of CFSAC attending the September 14 ICD-9-CM Coordination and Maintenance Committee meeting if it were permissible for CFSAC to give public testimony to another advisory body; Dr Jones stated that she would check the rules. Medical attorney, Steven Krafchick, had been particularly keen to see this suggestion taken forward.
Coalition4ME/CFS initiative
In a Press Release dated September 12, 2011, the Coalition4ME/CFS, which comprises a number of US 501 (c)(3) registered ME and CFS organizations, announced that the Coalition had submitted a representation to NCHS in July.
The Coalition had set out its proposals and a rationale in a 48 page letter dated July 14 and had been successful in getting the issue of the proposed coding of CFS in ICD-10-CM placed on the agenda for the September 14 meeting of the ICD-9-CM Coordination and Maintenance Committee.
Mary Dimmock and Marly Silverman attended the September meeting and presented the Coalition’s proposal and rationale to the NCHS. The NCHS presented an alternative suggestion to the current proposal for the coding of CFS in ICD-10-CM on which stakeholders may also wish to submit comment.
The Coalition4ME/CFS’s materials can be found here:
There are a quite a number of background documents on the Coalition’s site and you may want to start with the Coalition’s Summary and Overview document.
You’ll also find the Coalition’s Press Release, ICD FAQ, Coalition Proposal, ICD Presentation (PPT), ME-ICC Update, ICD Meeting Update, IACFS Conference info and an ICD Sample Letter (a template for submitting comment to NCHS in support of the Coalition’s proposals).
What is the Coalition4ME/CFS proposing?
The Coalition proposes that for ICD-10-CM, Chronic fatigue syndrome (currently coded as “Chronic fatigue syndrome NOS”) should be deleted from Chapter 18: R53.82 Malaise and fatigue and instead, classified within Chapter 6 Diseases of the nervous system under the parent class G93 Other diseases of brain, under the Title term G93.3 Postviral fatigue syndrome, under which code Benign myalgic encephalomyelitis is proposed to be classified.
• This would bring the US specific ICD-10-CM in line with international ICD-10 (in which CFS is indexed to G93.3) and ICD-10-CA (Canada), where all three terms are classsified within the ICD-10-CA Tabular List under G93.3.
• This would reflect the CFSAC Committee’s Recommendation to HHS of May 2011 which had prompted the Coalition’s initiative.
• This would bring ICD-10-CM in line with ICD-11, for which it is proposed that all three terms are classified in Chapter 6 Diseases of the nervous system.
I shall be setting out the various proposals in a forthcoming post.
September 14 Coordination and Maintenance Committee meeting
The CDC webpage for the development of ICD-10-CM is here: http://www.cdc.gov/nchs/icd/icd10cm.htm
The 2011 release for the draft ICD-10-CM is available from the page above under this section of the page. Note that although this release of ICD-10-CM is available for public viewing, the codes in ICD-10-CM are not currently valid for any purpose or use. The most recent update to the draft, the “2011 release of ICD-10-CM” replaces the December 2010 release.
The CDC webpage for the ICD-9-CM Coordination and Maintenance Committee remit, meeting schedules and meeting documentation is here: http://www.cdc.gov/nchs/icd/icd9cm_maintenance.htm
The ICD-9-CM Coordination and Maintenance Committee is a Federal Committee; suggestions for new inclusions to ICD-9-CM and modifications to proposals for the forthcoming ICD-10-CM come from both the public and private sectors. Interested parties and stakeholders are required to submit proposals for modification prior to a scheduled meeting.
These twice yearly meetings are held as public fora to discuss proposed modifications to ICD-9-CM and proposals for ICD-10-CM and a number of proposals and modifications around other diseases and disorders had been tabled for discussion on September 14, in addition to the issue of the coding of CFS in ICD-10-CM.
Meeting presentation
Mary Dimmock (who prepared the proposal) and Marly Silverman (PANDORA founder and Coalition4ME/CFS steering committee member) presented on behalf of the Coalition at the NCHS’s September 14 meeting.
At the meeting, the NCHS had presented an alternative suggestion to the current proposal for the coding of CFS in ICD-10-CM which suggested coding (B) ME and CFS under two separate sub codes (G93.31 and G93.32) under a revised G93.3 parent “G93.3 Postviral and other chronic fatigue syndromes” (a not entirely satisfactory suggestion that I shall set out in full in a forthcoming post). I shall be posting extracts from the two NCHS meeting Proposals and Summary documents where they relate to the issue of the coding of CFS in the next post, and you can download the entire documents from the links below.
You can download an Audio of the September 14 NCHS meeting here: http://www.cms.gov/ICD9ProviderDiagnosticCodes/Downloads/091411_Meeting_Audio.zip
[Note this is a large Zipped file. The section for discussions on CFS coding starts at 2 hours 27 minutes in from start and ends at 3 hours 02 minutes.]
The NCHS Committee’s Summary of the proceedings of this meeting can be downloaded here: Summary September 14, 2011. See Page 2.
The CDC site says, “Note: This document was re-posted, changes are on page 2, bullet 2, bolded. If you downloaded the previous document you will need to download this updated document.”
The NCHS Committee’s Proposals document is here: Proposals September 14, 2011. See Pages 10-11.
The CDC site says, “Note: This document was re-posted, if you downloaded the previous document you will need to download this updated document.”
What’s the deadline for comments and where do I send them?
The closing date for submitting comments to NCHS on the proposals is Friday, November 18.
Comments from stakeholders, preferably via email, should be submitted to:
Donna Pickett RHIA, MPH
Medical Classification Administrator
National Center for Health Statistics – CDC
3311Toledo Road Hyattsville, MD 20782
Via email: nchsicd9CM@cdc.gov
Coming up…
In upcoming posts I’ll be setting out the various proposals and the NCHS’s suggestion, for ease of comparison, and a posting by Mary Schweitzer around ICD-10-CM.
Footnotes and related postings:
1] Minutes of May 10-11 2011 CFSAC meeting (Extract: Discussion of concerns re coding of CFS for ICD-10-CM)
2] A Summary of Chronic Fatigue Syndrome and Its Classification in the International Classification of Diseases CDC, 2001.
3] CFS orphaned in the “R” codes in US specific ICD-10-CM
4] Forthcoming US “Clinical Modification” ICD-10-CM (starts half way down page)
5] I have written to the CDC’s, Donna Pickett, to request that consideration is given to posting stand alone PDFs of the draft Tabular List and Index. (At the moment, these two documents require extraction or opening in situ from a 14 MB Zipped file which contains five PDFs, which include the ICD-10-CM Tabular List and the Alphabetical Index.)
To view or download the Tabular List and Alphabetical Index for the 2011 release of ICD-10-CM:
Go to: http://www.cdc.gov/nchs/icd/icd10cm.htm#10update
Heading: ICD-10-CM Files – 2011 release
Click on: ICD-10-CM PDF Format for which the URL is
ftp://ftp.cdc.gov/pub/Health_Statistics/NCHS/Publications/ICD10CM/2011/
Open or save this directory file:
12/20/2010 08:40AM 14,131,267 icd10_cm_pdf.zip
contains 5 PDF files, which include the Tabular List (7.8 MB) and the Alphabetical Index (4.7 MB) which can be viewed in situ or saved to hard drive.