Proposals for the classification of Chronic pain in ICD-11: Part 1
August 22, 2015
Post #325 Shortlink: http://wp.me/pKrrB-488
Part 1
In 2013, the International Association for the Study of Pain (IASP) launched a working group tasked with developing proposals for the classification of chronic pain within ICD-11, for application in primary care, low-resource environments and clinical settings for specialized pain management.
The Classification of Chronic Pain Task Force is working under the auspices of WHO/ICD Revision. The group is co-chaired by IASP President, Prof. Dr. med. Rolf-Detlef Treede, and Winfried Rief PhD, Professor of Clinical Psychology and Psychotherapy, University of Marburg.
The working group held its first meeting in March 2013. At that point, the potential for creating a new Pain chapter in ICD-11 was reportedly under consideration (Organizing Principles, Classifying pain for healthcare, Carol Cruzan Morton, April 2013).
But the concept of a dedicated pain chapter for ICD-11 appears to have been set aside in preference to expanding the existing Chronic pain classification within the Symptoms, signs, clinical forms, and abnormal clinical and laboratory findings, not elsewhere classified chapter (currently numbered Chapter 21 in the Beta draft).
Under this new Chronic pain disorder section, “…diagnoses in which pain is either the sole or a leading complaint of the patient will be listed.”
Additionally, chronic pain conditions considered neglected in previous ICD versions, for example, chronic cancer pain, chronic neuropathic pain and chronic visceral pain, will be represented under Chronic pain with their own codes.
A simplified version of the proposed framework for use by primary care practitioners was expected to undergo field testing in several countries. A more detailed specialty ICD-11 linearization for use by pain specialists is also envisaged.
What are the most recent proposals from the IASP Chronic Pain Task Force?
In March 2015, the IASP working group published a paper setting out proposals and rationales for the structure of a new Chronic pain section and the disorders classified within it.
Initially, the paper was behind a paywall, but was published under Open Access in June 2015. You can read the paper in html and PDF format here:
A classification of chronic pain for ICD-11. Rolf-Detlef Treede, Winfried Rief et al
Pain. 2015 Jun; 156(6): 1003-7. Published online 2015 Mar 14. PMCID: PMC4450869
Under the proposed framework, chronic pain will be defined as pain that persists or recurs for more than three months.
There are optional specifiers for each diagnosis for recording evidence of psychosocial factors and pain severity. Pain severity can be graded on the basis of pain intensity, pain-related distress, and functional impairment.
“Detailed Explanation of the Proposal” texts for Chronic pain and its 7 child categories have been uploaded to the ICD-11 Beta draft Proposals Mechanism on behalf of the working group.
These are important texts setting out detailed proposals, rationales and criteria and are open for review, comment and suggestions for changes, for which registration with the Beta draft is required. There are links for these texts below but for ease of reference, I am including selected of these texts in .doc format.
Proposed disorder categories
The new ICD section for Chronic pain is proposed to comprise the most common clinically relevant disorders, divided into 7 groups (Fig. 1, Treede et al, 2015).
Chapter 21: Symptoms, signs, clinical forms, and abnormal clinical and laboratory findings, not elsewhere classified
General symptoms, findings and clinical forms
General symptoms
(…)
Pain
Chronic pain [Detailed Proposals] [.doc document]
Update: Proposals for Chronic pain replaced with [Detailed Proposals] Antonia Barke 17.09.15
2.1. Chronic primary pain [Detailed Proposals] [.doc document]
Subclass: Mono-site primary chronic pains syndromes [Detailed proposals not available]
Subclass: Multi-site primary chronic pains syndromes [Detailed proposals not available]
Fibromyalgia [Detailed proposals not available]
2.2. Chronic cancer pain [Detailed Proposals]
2.3. Chronic postsurgical and posttraumatic pain [Detailed Proposals]
2.4. Chronic neuropathic pain [Detailed Proposals]
2.5. Chronic headache and orofacial pain [Detailed Proposals]
2.6. Chronic visceral pain [Detailed Proposals] [.doc document]
2.7. Chronic musculoskeletal pain [Detailed Proposals] [.doc document]
According to its Detailed Proposals text, Chronic primary pain is proposed to be primary parented under Chronic pain and secondary parented to Diseases of the nervous system.
Other chronic pain disorders are proposed to be primary parented under Chronic pain and secondary parented to Neoplasms, Diseases of the nervous system, Diseases of the respiratory system, Diseases of the digestive system, Diseases of the musculoskeletal system and connective tissue or Diseases of the genitourinary system, according to body system.
The “Appendix Structure of the chapter on chronic pain” (page 4 of the Treede et al paper) sets out a complex hierarchy of subclasses.
It’s not evident whether all or selected of these additional subclasses are intended to be added under the disorder categories that are currently displaying in the Beta draft, or whether additional subclasses would be reserved for use in a specialist linearization for chronic pain.
The Treede et al paper describes Chronic primary pain as:
2.1. Chronic primary pain
Chronic primary pain is pain in 1 or more anatomic regions that persists or recurs for longer than 3 months and is associated with significant emotional distress or significant functional disability (interference with activities of daily life and participation in social roles) and that cannot be better explained by another chronic pain condition. This is a new phenomenological definition, created because the etiology is unknown for many forms of chronic pain. Common conditions such as, eg, back pain that is neither identified as musculoskeletal or neuropathic pain, chronic widespread pain, fibromyalgia, and irritable bowel syndrome will be found in this section and biological findings contributing to the pain problem may or may not be present. The term “primary pain” was chosen in close liaison with the ICD-11 revision committee, who felt this was the most widely acceptable term, in particular, from a nonspecialist perspective.
and (under 2.7. Chronic musculoskeletal pain):
…Well-described apparent musculoskeletal conditions for which the causes are incompletely understood, such as nonspecific back pain or chronic widespread pain, will be included in the section on chronic primary pain.
Under two new terms: Mono-site primary chronic pains syndromes and Multi-site primary chronic pains syndromes the IASP working group proposes to locate irritable bowel syndrome; chronic nonspecific back pain; chronic pelvic pain; chronic widespread pain; fibromyalgia, and potentially some other conditions where chronic pain is a feature.
This “new phenomenological definition” appears to be an umbrella diagnosis for a number of the so-called, “functional somatic syndromes.”
There is a considerable amount of psychosomatics in the Detailed Proposals document for Primary chronic pain.
It is unclear whether the intention is to add discrete categories for irritable bowel syndrome; chronic nonspecific back pain; chronic widespread pain, and other diagnoses proposed to be aggregated under the Chronic primary pain term. But at the time of compiling this report, Fibromyalgia is the only term to have been inserted.
In the ICD-11 Beta draft, Irritable bowel syndrome remains at its current location in Diseases of the digestive system chapter, under Irritable bowel syndrome and certain specified functional bowel disorders.
It is therefore unclear whether the ICD-11 Revision Steering Group and the IASP working group have reached consensus over the proposed relocation of Irritable bowel syndrome to the Symptoms, signs chapter, under a new Chronic primary pain parent.
I have requested clarification of current intentions for Irritable bowel syndrome via the Proposal Mechanism comments facility but have received no response.
Proposed new ICD-11 categories
These are the disorder categories as currently entered into the ICD-11 Beta drafting platform under parent class: Pain > Chronic pain for the Foundation Component:

ICD-11 Beta drafting platform, public version: Foundation Component. Accessed August 20, 2015.
A note about discrepancies in terminology between ICD-11 Beta draft and the Treede et al paper: The term, Primary chronic pain, as entered into the Beta draft, is proposed to be amended to Chronic primary pain, in line with the classification structure set out in Table: Appendix Structure of the chapter on chronic pain on page 4 of the Treede et al paper.
The Beta draft’s Mono-site primary chronic pains syndromes and Multi-site primary chronic pains syndromes are termed Localized chronic primary pain (including nonspecific back pain, chronic pelvic pain) and Widespread chronic primary pain (including fibromyalgia syndrome) in the Treede et al paper.
(I have also enquired whether the Mono- and Multi-site primary chronic pains syndromes terms are to be amended to Mono- and Multi-site chronic primary pain syndromes but have received no response.)
If you are a stakeholder in any of the terms proposed to be classified under this new Symptoms, signs chapter section, please scrutinize the IASP Task Force paper and the Detailed Proposals documents and bring these proposals to the attention of your patient organizations.
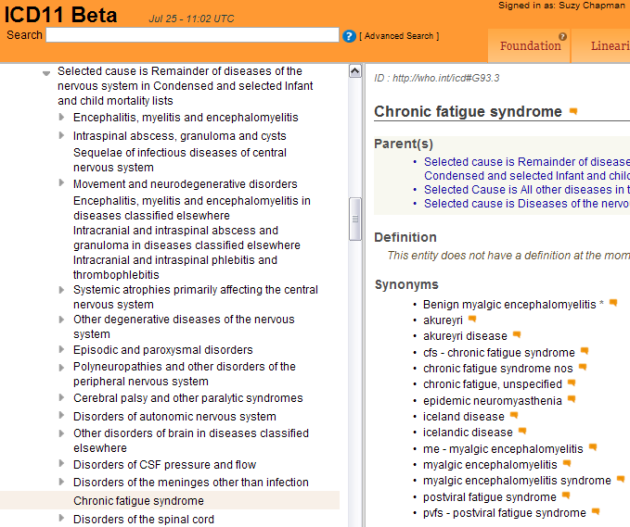
The G93.3 legacy terms: Postviral fatigue syndrome; Benign myalgic encephalomyelitis; Chronic fatigue syndrome
I have no documentary evidence of intention to locate any of the ICD-10 G93.3 legacy terms under this proposed Symptoms, signs chapter Chronic pain > Chronic primary pain section.
WHO’s, Dr Robert Jakob, told me in June 2015 that he expects TAG Neurology to release proposals and rationales for the classification of the G93.3 legacy terms in September or December, latest. See summary of discussions with WHO personnel, June 19, 2015 http://wp.me/pKrrB-46A
Update: Since no proposals and rationales for the ICD-10 G93.3 legacy terms were released in September or December 2015, I contacted ICD’s Dr Robert Jakob. I was told on February 2, 2016 that “[ICD-11 Revsion is] still working on the extensive review and the conclusions.”
Click here for Part 2 Fibromyalgia